CASE REPORT | https://doi.org/10.5005/jp-journals-10049-0062 |
Freeman–Sheldon Syndrome
1–3Department of Anaesthesiology, King Edward Memorial Hospital and Seth Gordhandas Sunderdas Medical College, Mumbai, Maharashtra, India
4Department of Anesthesiology, Topiwala National Medical College and BYL Nair Charitable Hospital, Mumbai, Maharashtra, India
Corresponding Author: Abhilasha D Motghare, Department of Anaesthesiology, King Edward Memorial Hospital and Seth Gordhandas Sunderdas Medical College, Mumbai, Maharashtra, India, Phone: +91 9860819602, e-mail: abhilashamotghare@gmail.com
How to cite this article Motghare AD, Kharge ND, Meshram SA, et al. Freeman–Sheldon Syndrome. Res Inno in Anesth 2019;4(1):19–20.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Freeman–Sheldon syndrome1 is a rare progressive myopathic disorder. The presence of difficult airway, poor venous access, and possible susceptibility to malignant hyperthermia make anesthesia management challenging in these patients.2 We report the case of a child with Freeman–Sheldon syndrome with microstomia posted for posterior release of clubfoot.
Keywords: Anesthesia, Difficult airway, Freeman–Sheldon syndrome, Microstomia.
CASE DESCRIPTION
A 5-year-old male child, weight 10 kg, height 89.5 cm, presented to a tertiary care center for bilateral posterior release for congenital talipes equinovarus (CTEV) (Fig. 1).
On clinical examination, he had facial dysmorphism (Figs 2 and 3)—flat occiput, low-set ears, widely spaced eyes, flat nose, midfacial hypoplasia, congenital left-sided facial palsy, and absent nasolabial folds. Oral examination showed microstomia—mouth opening of 1 cm, poorly formed teeth, and high-arched palate. He had a deviated nasal septum with hypertrophied adenoids and also intermittent snoring episodes at night and also had global developmental delay. Patient’s mother gave history of running nose and cough a day prior to surgery. On further history, it was found that he had undergone some surgery for CTEV under general anesthesia, the details of which were not available. He had MRI of the brain done few days back under general anesthesia, which revealed brachycephaly. Both the anesthesia exposures were uneventful.
The blood investigations and echocardiography were within normal range. The child was started on nebulization and intravenous (IV) antibiotics prior to surgery. A valid informed consent was taken from the parents and all the risk were explained to them in the language they understood. A pediatric ICU bed was kept booked for this patient. We were anticipating a difficult airway, so the difficult airway cart was kept ready.

Fig. 1: Characteristic features of Freeman–Sheldon syndrome
The child was allowed clear liquids 2 hours prior to surgery. He had received nebulization and IV antibiotics in the wards.
Since an IV line was in situ, we proceeded with IV induction. He received inj. midazolam 1 mg in the preoperative room and once he was calm and quiet was shifted to the operating room. The standard anesthesia monitors were attached and then inj. fentanyl 20 μg, inj. propofol 30 mg, and inj. atracurium 5 mg (after confirmation of mask ventilation) were given. After adequate muscle relaxation, laryngoscopy was done using CMAC videolaryngoscope Miller blade 1. The Cormac Lehane was grade I and he was intubated with 4.0 uncuffed ETT. The anesthesia was maintained with oxygen, air, and sevoflurane to maintain MAC 1. For analgesia, a caudal block with 5 mL of 0.25% bupivacaine with 20 μg of clonidine was given. The patient developed bronchospasm with peak inspiratory pressure up to 36 cm of H2O and relieved after steroid and salbutamol puff. The surgery lasted for 6 hours with minimal blood loss. All the monitored vitals and temperature were stable throughout the procedure. At the end of the procedure, the child was extubated uneventfully and then shifted to the recovery room for observation and subsequently to wards.
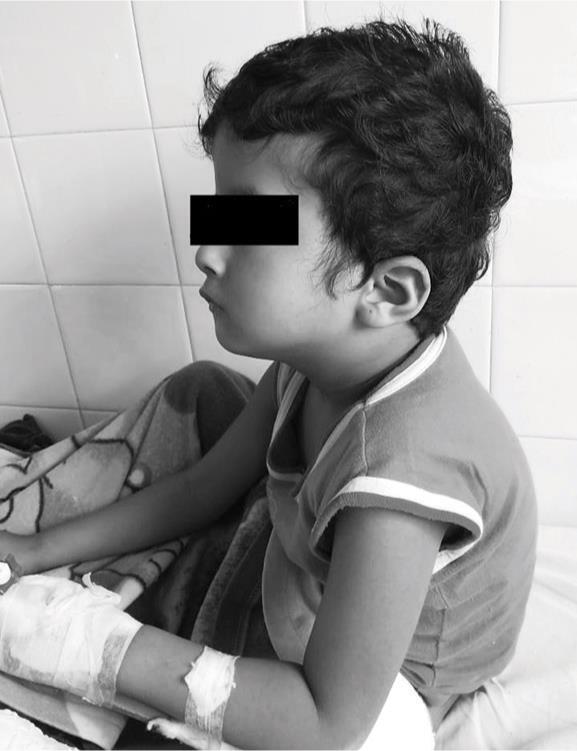
Fig. 2: Facial dysmorphism (low set ears) in side view
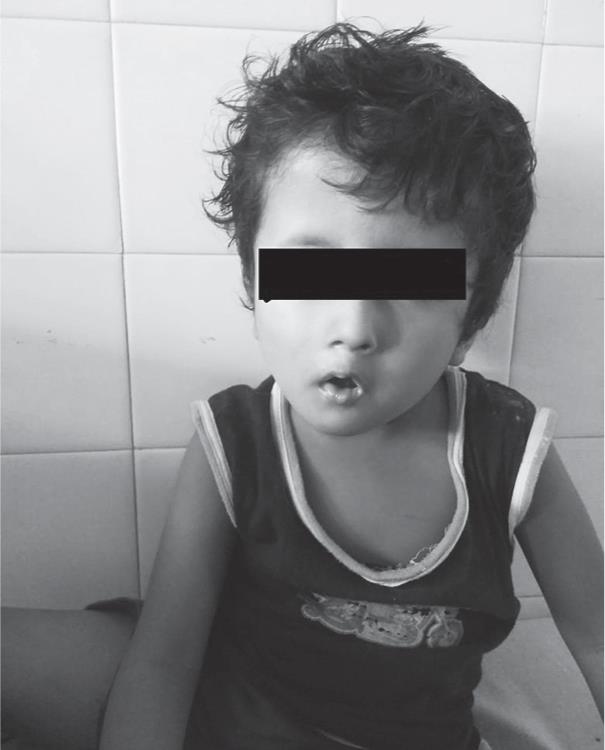
Fig. 3: Facial dysmorphism (microstomia) in front view
DISCUSSION
Freeman–Sheldon syndrome, a slowly progressive congenital myopathy, usually presents with multiple body contractures, skeletal malformations, and craniofacial deformities such as microstomia, micrognathia, microglossia, a high-arched palate, and midfacial hypoplasia characteristically known as whistling mouth syndrome.3 These patients undergo multiple orthopedic, soft tissue, and cosmetic surgeries for improving quality of life and hence multiple anesthesia exposures. Keeping in mind the difficult airway and the risk of malignant hyperthermia, the anesthesia management becomes challenging. Also the patients are prone for respiratory complications. Hence, we shared the experience of managing this syndromic child. Some studies have used laryngeal mask airway and regional anesthesia for management.3,4 Our patient had limited mouth opening that took Millers 1 blade and we were able to intubate. But everything anticipating difficult airway was kept ready. Also previous anesthesia exposure was uneventful, so there was less risk of malignant hyperthermia in subsequent anesthetics.5 But we have flushed the machine a day prior to surgery, changed soda lime, and taken a new closed circuit. Cold saline was kept ready. Dantrolene sodium, if needed, was available from a nearby corporate hospital. The anesthesia technique and the complications encountered have been mentioned in the literature.2
REFERENCES
1. Gurjar V, Parushetti A, Gurjar M. Freeman-Sheldon syndrome presenting with microstomia: a case report and literature review. J Maxillofac Oral Surg 2013 Dec;12(4):395–399. DOI: 10.1007/s12663-012-0392-4.
2. Bosenberg A. Anesthesia and Freeman Sheldon Syndrome. South Afr J Anaesth Analg 2003; 17–19.
3. Patel K, Gursale A, Chavan D, et al. Anesthesia challenges in Freeman-Sheldon syndrome. Indian J Anaesth 2013;57(6):632–633. DOI: 10.4103/0019-5049.123352.
4. Cruickshanks GF, Brown S, Chitayat D. Anesthesia for Freeman-Sheldon syndrome using a laryngeal mask airway. Can J Anaesth 1999;46:783. DOI: 10.1007/BF03013916.
5. Mayhew JF. Anesthesia for children with Freeman Sheldon Syndrome. Anaesthesiology 1993;78:408. DOI: 10.1097/00000542-199302000-00042.
________________________
© The Author(s). 2019 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.